Lymphedema & Phlebolymphedema
Lymphedema & Phlebolymphedema
Understanding and Management
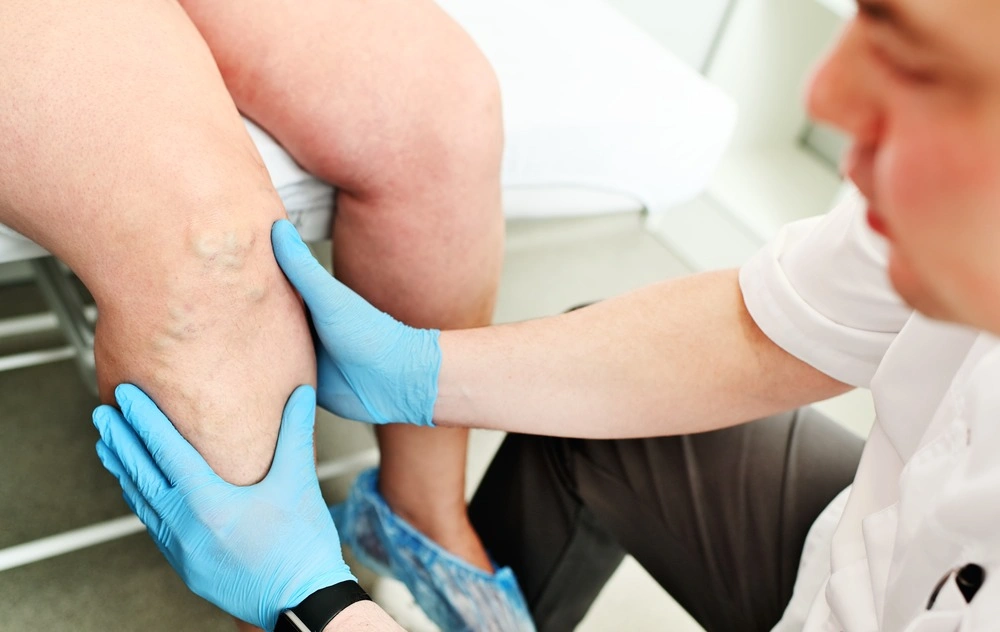
Lymphedema & Phlebolymphedema Q & A
What is Lymphedema?
What causes Lymphedema?
The lymphatic system is a network of vessels that carry protein-rich lymph fluid throughout the body. It’s part of your immune system. Lymph nodes act as filters and contain cells that fight infection and cancer.
The lymph fluid is pushed through the lymph vessels by muscle contractions as you move through the tasks of your day and small pumps in the wall of the lymph vessels. Lymphedema occurs when the lymph vessels are not able to adequately drain lymph fluid, usually from an arm or leg.
The most common causes of lymphedema include:
-
Cancer
If cancer cells block lymph vessels, lymphedema may result. For instance, a tumor growing near a lymph node or lymph vessel could enlarge enough to block the flow of the lymph fluid. -
Radiation Treatment for Cancer
Radiation can cause scarring and inflammation of lymph nodes or lymph vessels. -
Surgery
In cancer surgery, lymph nodes are often removed to see if the disease has spread. However, this doesn’t always result in lymphedema. -
Parasites
In developing countries in the tropics, the most common cause of lymphedema is infection with threadlike worms that clog the lymph nodes.
What symptoms develop due to Lymphedema?
- Swelling of part or all of the arm or leg, including fingers or toes
- A feeling of heaviness or tightness
- Restricted range of motion
- Recurring infections
- Hardening and thickening of the skin (fibrosis)
- Signs and symptoms can range from mild to severe. Lymphedema caused by cancer treatment may not occur until months or years after treatment.
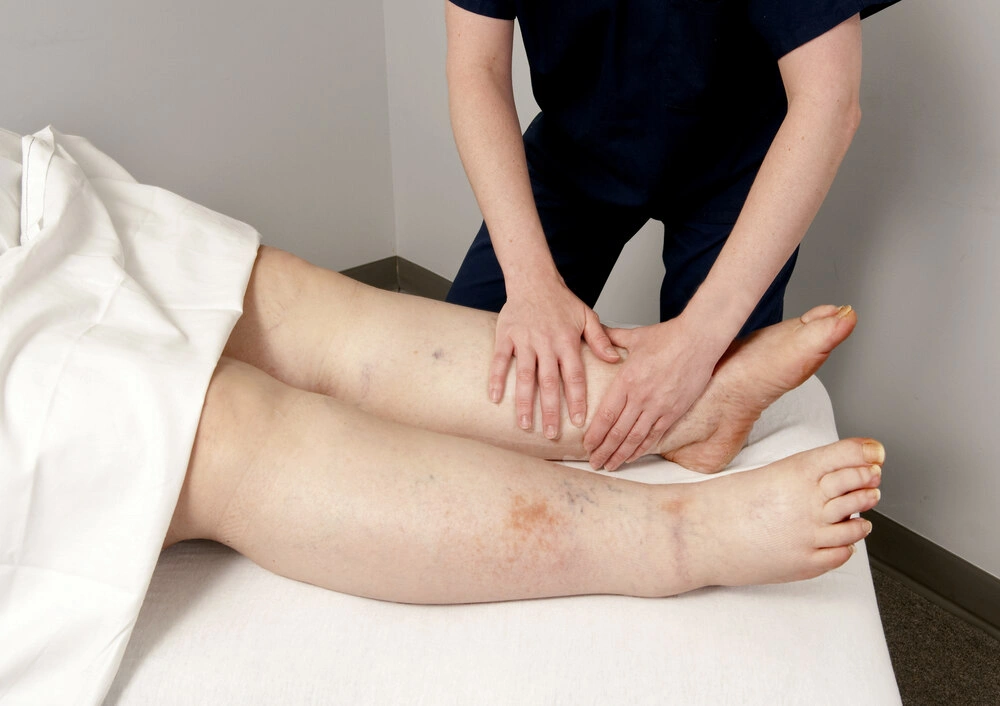
How is Lymphedema Treated?
-
Medications:
Lymphedema greatly increases the risk of skin infections (cellulitis). Your doctor may prescribe antibiotics for you to keep on hand so that you can start taking them immediately once symptoms appear. -
Therapy:
Specialized lymphedema therapists can teach you about techniques and equipment that can help reduce lymphedema swelling. Examples include:
- Exercises. Gentle contraction of the muscles in the arm or leg can help move the excess fluid out of the swollen limb.
- Manual lymph drainage. Therapists trained in this massage-like technique use very light pressure to move the trapped fluid in the swollen limb toward an area with working lymph vessels. People should avoid manual lymph drainage if they have a skin infection, blood clots or active cancer in the affected limb.
- Compression bandages. Using low-stretch bandages to wrap the entire limb encourages lymph fluid to flow back toward the trunk of the body.
- Compression garments. Close-fitting elastic sleeves or stockings can compress the arm or leg to encourage lymph fluid drainage. These garments often require a prescription to ensure that the proper amount of compression is used. You may need to be measured by a professional to ensure proper fit.
- Sequential pneumatic compression. A sleeve worn over the affected arm or leg connects to a pump that intermittently inflates the sleeve, putting pressure on the limb and moving lymph fluid away from the fingers or toes.
Surgical and Other Procedures
- Lymph node transplant. Lymph nodes are taken from a different area of the body and then attached to the network of lymph vessels in the affected limb. Many people with early-stage lymphedema see good results from this surgery and can decrease the amount of compression needed.
- New drainage paths. Another option for early-stage lymphedema, this procedure creates new connections between the lymph network and blood vessels. The excess lymph fluid is then removed from the limb via blood vessels.
- Removal of fibrous tissue. In severe lymphedema, the soft tissues in the limb become fibrous and hardened. Removing some of this hardened tissue, often through liposuction, can improve the limb's function. In very severe cases, hardened tissue and skin may be removed with a scalpel.
Informational PDFs
Phlebolymphedema
What is Phlebolymphedema?
Phlebolymphedema is the most common form of lymphedema in the Western world. It is a combined lymphatic and vascular condition that causes inflammation and lymphedema in the feet and lower legs. It begins with chronic venous insufficiency (CVI) in which the one-way valves in the veins of the lower legs lose the ability to completely close.
While most of the blood normally moves upwards back to the heart, some blood flows backwards because of the faulty valves.
This backward flow, called venous reflux, strains the vein walls and blood plasma leaks into the interstitial space. This produces swelling in the feet, ankles, and calves. The lymphatic system works as a safety valve to move the excess fluid out of the legs.
CVI usually affects both legs. At first, CVI symptoms might show up as swollen ankles at the end of the day that reduce overnight when legs are horizontal in bed. As CVI becomes more advanced, it causes lymphatic overload and becomes phlebolymphedema.
What causes Chronic Venous Insufficiency (CVI) and Phlebolymphedema?
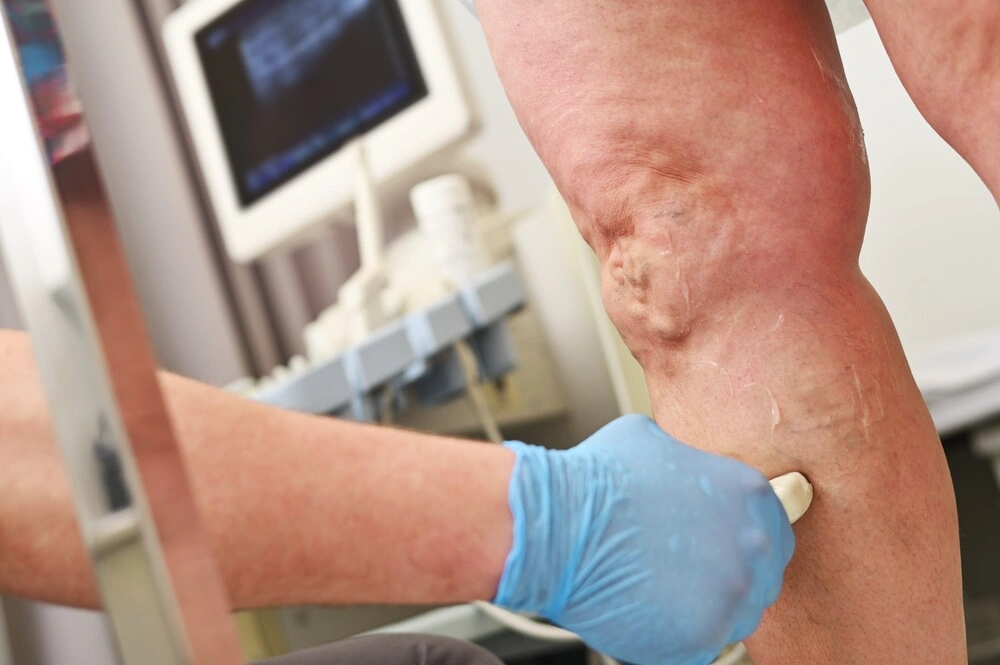
What symptoms develop due to Phlebolymphedema?
- Brownish-bronze areas are known as hyperpigmentation or hemosiderin staining. This brown discoloration is caused by red blood cells leaking out of the veins and permanently staining the skin.
- Hardened brown patches can appear after a cellulitis infection.
- Star-shaped white scars called atrophie blanche are sometimes left after an infection or healed ulcer.
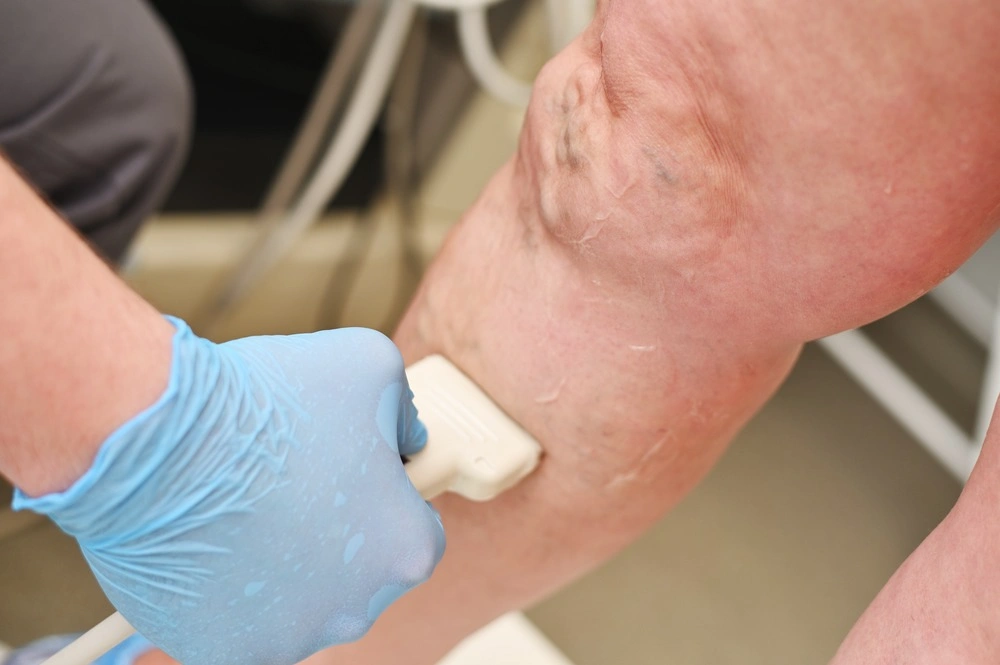
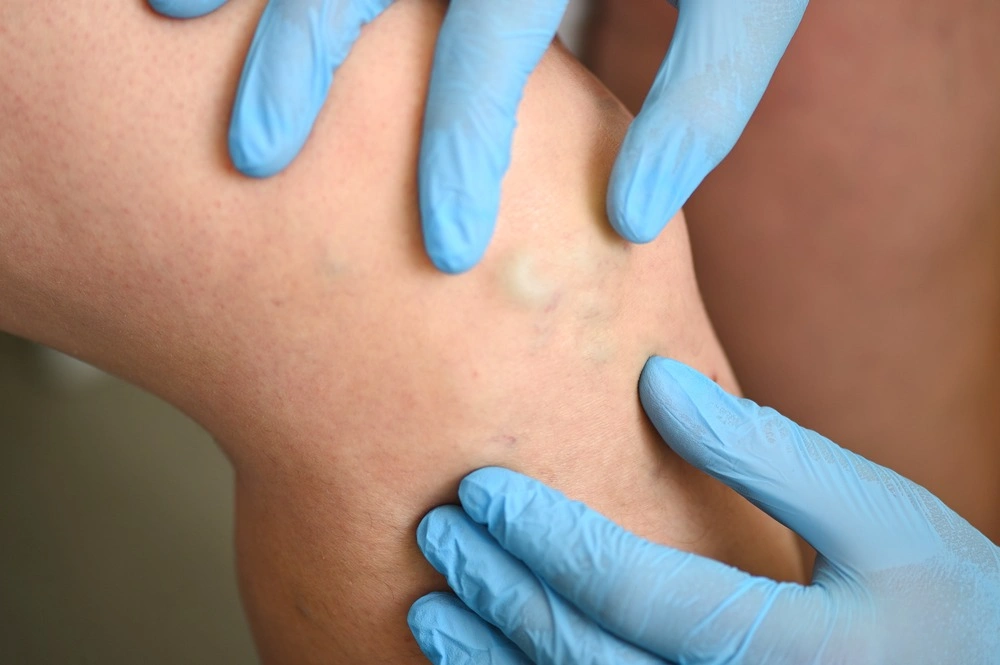
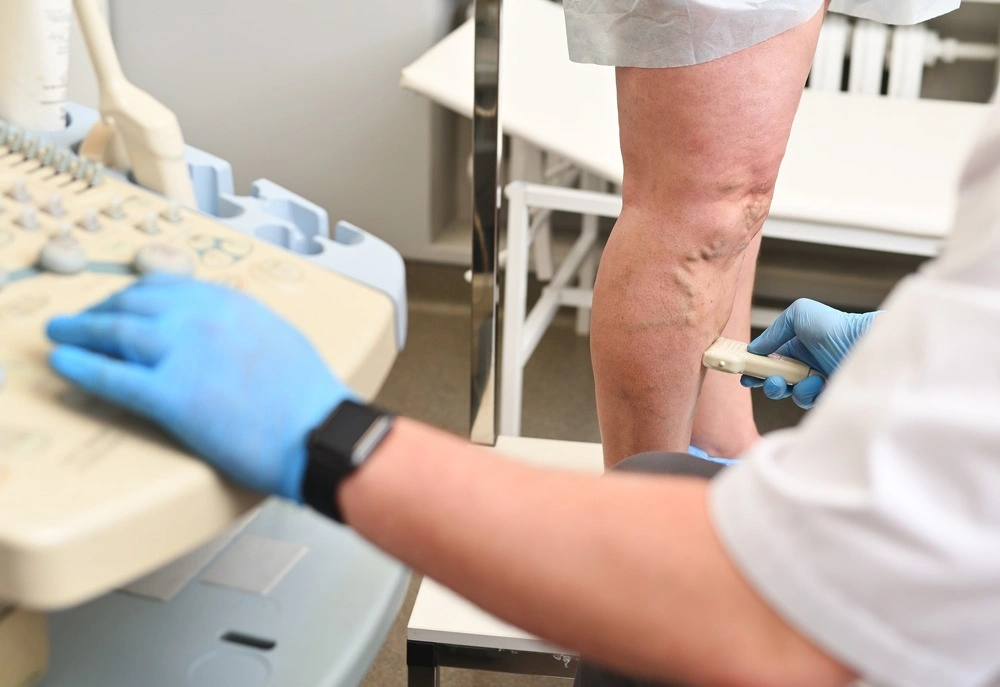
- Purple varicose veins are visibly enlarged and may be painful. Small red-purple broken venules are called telangiectasia (spider veins.)
- Redness with normal leg temperature that resolves with elevation can be due to vasodilation.
- Redness with heat can be caused by erythema, which is a form of inflammation.
- Red-purple discoloration around the ankles that is accompanied by itching, sores and thickened skin can signal stasis dermatitis.
How is Phlebolymphedema Treated?
It is important for patients to have a comprehensive treatment program to reduce swelling and prevent progression of phlebolymphedema. Patients with phlebolymphedema benefit from treatment by wound care specialists and by certified lymphedema therapists.
Complete decongestive treatment is administered by a certified lymphedema therapist. This treatment consists of manual lymphatic drainage, compressive wraps and garments, skin care, and exercise. Conservative treatment consists of elevation, exercise, and compression.
Manual lymphatic drainage is a specialized type of medical massage that increases vascular and lymphatic circulation, and decongests swelling. Modification may be necessary for patient comfort if there is a painful wound present.
Areas of heavy fibrotic damage require more pressure against the surface of dense tissue in order to effectively move swelling that is trapped inside and underneath. Applying compression following manual lymphatic drainage is important to maintaining the reduction of swelling.
Wearing compression on the feet and legs helps swelling in a number of ways. External pressure that compresses against the veins improves their ability to move blood upward. This pressure also helps the lymph system. Wearing compression during exercise increases the effectiveness of the calf muscle pump.
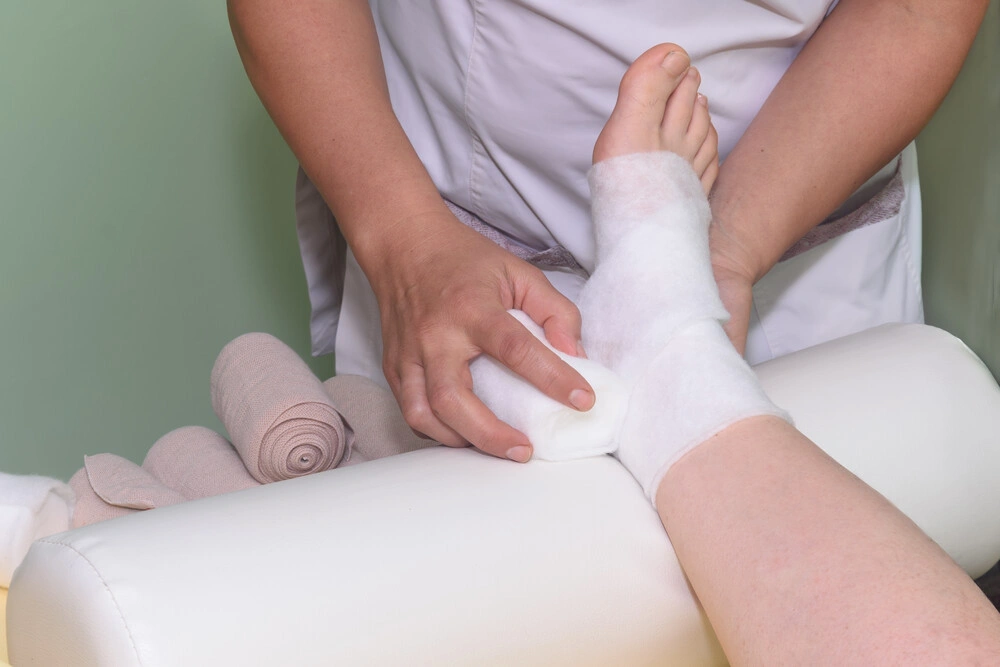
Layered bandages or Velcro compression wraps are used in the initial reduction phase of treatment for very swollen feet and legs. They are also used for those with wounds, or for those who have difficulty putting on tight compression stockings. Wound clinics often use disposable compression systems such as zinc oxide wraps or multi-layered Coban wraps over dressings.
Gradient elastic stockings are the most common form of compression. They are generally used in the maintenance phase of treatment. Ready-made stockings have greater pressure at the ankle that lessens towards the top of the stocking, but less pressure in the foot. Custom stockings, wraps, or even tight lace up shoes provide extra compression required for stubborn foot swelling.
First and foremost, all wounds must be treated. Because patients with phlebolymphedema are particularly vulnerable to wounds, prevention is critical. Dry, cracked, and itchy skin is common with phlebolymphedema. Moisturizing the skin heals these symptoms and builds a better barrier to avoid infections.
Walking utilizes the pumping action of the calf muscles to improve circulation in the veins and lymphatic vessels. Even seated exercise can be helpful. Doing ankle pumps for one minute can increase circulation in the legs for thirty minutes.
Ankle flexibility is crucial for proper calf muscle contraction. With tight ankles the calf muscles can’t fully contract as we see in those who “shuffle” when they walk. These people struggle more with swelling because the calf muscle pump is impaired. Those with paralysis or weakness of the lower legs are particularly vulnerable to swelling, however upper body exercise can help increase overall body circulation.
For those without wounds, aquatic exercise gives the benefit of water compression, making muscle contraction more effective. The deeper the water, the better because of greater compression at greater depth: For example, three feet of water creates 67.26 mmHg of pressure on the feet.
Deep abdominal breathing during exercise is also important to activate the diaphragmatic pump, which increases overall blood and lymph circulation.
Elevating the legs uses gravity to help move blood toward the heart. It also assists in the movement of lymph fluid to the lymph nodes in the back of the knees and the groin. These lymph nodes process and filter the fluid so it can eventually exit the body as urine.
Changing the position of the legs from time to time during the daytime is important. Many patients find it helpful to take an afternoon rest in bed with legs elevated on pillows. Some have difficulty lying flat on a bed because of back pain, sleep apnea, or other breathing issues, and prefer a recliner chair for sleep. However, most recliner chairs do not elevate legs horizontally to the level of the heart, leaving legs in a semi-dependent position. A hospital bed can help elevate both the upper body and the legs.